Bladder pain syndrome (interstitial cystitis) is a problem that causes pain in the bladder or pelvis. It also causes an urgent, frequent need to urinate. The problem is much more common in women than in men.To diagnose bladder pain syndrome (BPS), your doctor may do a test called cystoscopy that uses a thin, lighted tube to see the inside of your bladder. He or she may also do a urine test to rule out other problems, such as a urinary tract infection. Some doctors think BPS may be caused by abnormal changes in the lining of the bladder. But the cause isn’t clear. Because of this, treatment focuses on helping to relieve symptoms. Your doctor may have you use a bladder diary to record how often you urinate and about how much urine is released.
Interstitial Cystitis
Women’s Health Concerns
Urinary Incontinence
Bladder Cancer
Overactive Bladder (OAB)
InterStim Bladder Modulator
Chronic UTI’s
Interstitial Cystitis
Pelvic Pain
Pelvic Organ Prolapse
How Is It Diagnosed
Dr. Bankhead will evaluate you and discuss with you the best path forward. She has developed an Interstitial Cystitis Pathway with many treatment options that can be tailored to your symptoms and needs. Sometimes a cystoscopy is needed to look for ulcers. The average time to diagnose IC is approximately 2 years, because it mimics recurrent bladder infections. Many patients are given antibiotic after antibiotic, but they never improve.
IC is not a urinary tract infection, and it can’t be identified by a simple urinalysis or urine culture. Rather, it’s a diagnosis of exclusion, which means that it’s diagnosed only after a number of other conditions have been ruled out. We’ll first take a thorough history, then conduct a physical exam (including a pelvic exam, if it’s not too uncomfortable) and perform tests for infection, bladder stones, bladder cancer, kidney disease, multiple sclerosis, endometriosis, sexually transmitted diseases, and other disorders. The AUA guidelines also recommend an early assessment of pain, urinary frequency, and urine volume, to help evaluate the effectiveness of later treatments.
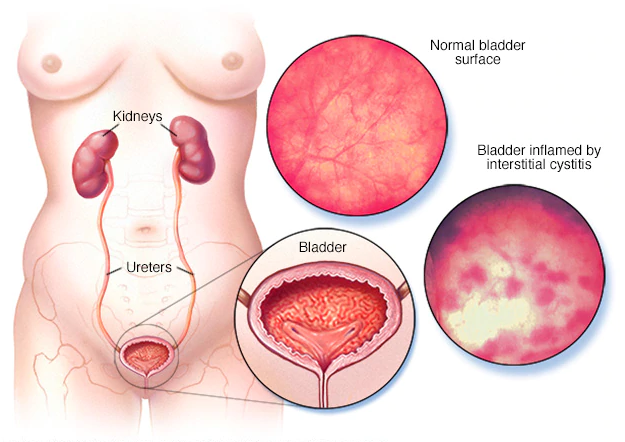
If a diagnosis is uncertain or there are symptoms (such as blood in the urine) that suggest other problems, the next step is usually cystoscopy, which involves inserting a fiber-optic tube through the urethra to look at the bladder wall. During the procedure, a tissue sample may be taken to rule out bladder cancer. Some physicians favor hydrodistention under local or regional anesthesia, which involves filling the bladder during cystoscopy with a liquid that stretches it, providing a closer view of the bladder wall. With IC, glomerulations — tiny pinpoint spots of blood — are usually visible on the bladder wall during cystoscopy with hydrodistention, but these lesions are often seen within the normal bladder as well.
One finding from cystoscopy that can help in making an IC diagnosis is the presence of reddened patches or lesions called Hunner’s ulcers, which can stiffen tissue and cause reduced bladder capacity. However, Hunner’s ulcers, which occur in 10% to 15% of cases, aren’t required to make an IC diagnosis.
What Are The Treatments?
Dietary changes. This is very important, because most patients have at least one triggering food or beverage. The biggest culprits are coffee, soda, tomatoes, citrus and spicy foods.
Stress reduction. While stress may not cause the condition, it definitely worsens it.
Physical therapy. A specialized pelvic floor physical therapist can work with you to relieve and resolve muscle spasm issues.
Muscle relaxants for the pelvic floor muscles around the bladder
Herbal supplements and acupuncture. While not mainstream, Dr. Bankhead has seen enough patients improve with these treatments that she does recommend them.
Prescription medications
Bladder instillations (putting medicine directly in the bladder)
Interstim therapy
Bladder or pelvic floor Botox
Urine DNA testing to look for evidence of bacteria in the bladder that normal testing does not detect.
Next Steps…
To schedule an appointment or to ask questions about anything we offer, give us a call at (405)942-8545, or click to message us.
